Serous tubal intraepithelial carcinoma detected during benign gynecologic surgery: a case report
Article information
Abstract
High-grade serous carcinoma (HGSC) is the most common type of pelvic cancer among women. Serous tubal intraepithelial carcinoma (STIC) is a precursor lesion of HGSC. Herein, we report a rare occurrence of STIC in patients undergoing surgery for benign indications without a family history of ovarian cancer. A 77-year-old woman underwent total laparoscopic hysterectomy and bilateral salpingo-oophorectomy for uterine prolapse. Pathological examination revealed bilateral STIC without ovarian abnormalities, and no other abnormal findings were noted. Another patient, a 49-year-old woman, underwent laparoscopic total hysterectomy and bilateral salpingectomy for uterine fibroids. STIC lesions were observed in both fallopian tubes. Subsequently, a staging was performed. No additional lesions were found, and the patient was followedup through imaging and blood tests. As reports of STIC lesions are rare, data on their clinical outcomes and management strategies are limited. In this report, we present cases of incidental STIC in benign surgery and discuss its proper interpretation and management. Through the early detection of STIC lesions, patients with risk factors can be identified in advance, which will allow prevention and early detection of ovarian cancer. Opportunistic salpingectomy was also actively discussed in this regard.
INTRODUCTION
High-grade serous carcinoma (HGSC) is the most common type of pelvic cancer among women and is responsible for most epithelial ovarian cancer-related deaths [1]. Since early detection through screening and symptoms has failed to reduce mortality, the only currently available strategy is prevention [2].
Our understanding of HGSC pathogenesis has substantially improved over the past few decades. Serous cancers are conventionally considered to originate from the ovarian surface epithelium or cortical inclusion cysts. The fallopian tubes have not been examined because ovarian carcinoma precursors are expected to arise from the ovaries. However, no ovarian precursor lesions have been identified. A hypothesis of malignant cell migration from the fallopian tube to the ovary has been proposed [2]. In women with a genetic predisposition for ovarian cancer, lesions closely resembling ovarian HGSC have been found in the fallopian tubes [3]. Histopathological evidence of risk-reducing salpingooophorectomy (RRSO) specimens and molecular genetic studies suggests that pelvic HGSCs frequently originate from fallopian tube precursor lesions, which are referred to as serous tubal intraepithelial carcinomas (STICs) [2].
With the discovery of HGSC originating from the fallopian tubes, alternative preventive strategies have emerged. In particular, prophylactic oophorectomy is performed in women at risk of ovarian cancer, and preventive measures involving the tube are now being considered. Thirteen members of the International Federation of Obstetrics and Gynecology society have stated guidelines regarding opportunistic salpingectomy, with the majority supporting this practice [3]. It will take decades to confirm the cancerreducing effect of salpingectomy, especially for the general population who undergo surgery for benign disorders.
A STIC diagnosis is rare in women undergoing salpingectomy for benign indications (<0.01%) [1]. Several studies have focused on high-risk patients who undergo RRSO in whom STICs are common. Currently, opportunistic salpingectomy is gradually being implemented; however, it is not easy to interpret benign STIC lesions and decide on an appropriate management strategy.
In this report, we present two cases of isolated STIC incidentally found during benign gynecological surgery, along with a brief literature review.
CASE REPORT
In the first case, the STIC was incidentally discovered during laparoscopic total hysterectomy and bilateral salpingo-oophorectomy for uterine prolapse correction.
A 77-year-old woman, gravida 4 para 4 (all delivered vaginally), presented to a hospital complaining of a recurrent vaginal bulge lasting 1 year. Pelvic organ prolapse quantification examination revealed stage-3 apical prolapse. No other unusual findings were observed on transvaginal ultrasonography. The patient had no significant medical or familial history of cancer. Total laparoscopic hysterectomy and bilateral salpingo-oophorectomy with sacral colopexy were performed. No significant intra-operative findings were observed. The uterus, bilateral tubes, and ovaries were sent for histopathological examination, and no gross abnormalities were noted in either specimen. The postoperative course was uneventful, and the patient was discharged on postoperative day 3. Pathological examination of the specimen revealed bilateral STIC (Fig. 1). Immunohistochemical staining showed a complete p53 loss. No pathological abnormalities were observed in either ovary. Management options, including close follow-up, secondary surgery for further evaluation with biopsy and staging, and empirical chemotherapy, were discussed with the patient. The patient decided to undergo observation and was followed-up with serial CA-125 estimation and imaging. To date, no such abnormalities have been reported.
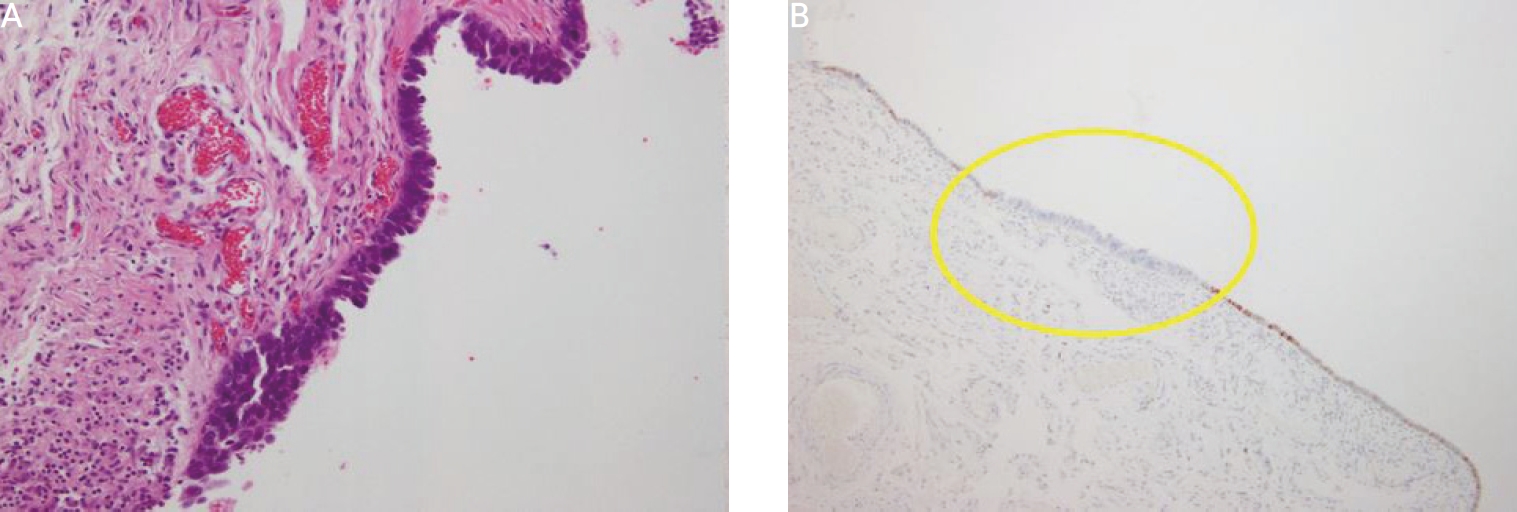
Histopathological findings of the specimen from the distal fallopian tube. (A) Stratified and thickened epithelial layer, focal loss of polarity and ciliated cells, lack of stromal invasion, enlarged nuclei, and hyperchromatic chromatin are visualized. Hematoxylin and eosin staining (×200). (B) Total negative expression of p53 was observed (in the yellow circle). Scattered nuclear stain (×200).
In the second case, the STIC was discovered after laparoscopic total hysterectomy and bilateral salpingectomy for uterine fibroids. A 49-year-old woman, gravida 1 para 1 (all delivered vaginally), was followed-up for multiple uterine fibroids on an outpatient basis. The patient underwent surgery, and three doses of gonadotropin-releasing hormone agonists were administered. The patient had no significant medical or familial history of cancer. Preoperative ultrasonography revealed no specific findings, other than the presence of uterine fibroids. Total laparoscopic hysterectomy and bilateral salpingectomy were performed; however, no significant intraoperative findings were observed. Pathological examination of the resected tissue revealed STIC in both fallopian tubes. Immunohistochemical staining revealed focal p53 positivity. These results were discussed with the patient; considering the potential risk, a staging operation was performed with bilateral oophorectomy. No specific findings were observed on the postoperative abdominopelvic computed tomography or positron emission tomography-computed tomography. The CA-125 level was 21.90, which was within the normal range. Laparoscopic bilateral oophorectomy, partial omentectomy, and right-sided round ligament resection were performed. Pathological examination revealed that the specimens were benign. The patient was discharged without complications, and follow-up imaging and blood tests were performed at an outpatient clinic.
This is a case report; therefore, the approval of the ethics committee and institutional review board was not required.
DISCUSSION
Approximately 20 years of progressive data accumulation has established that the distal fallopian tube is an origin site for HGSC, which was evident when STIC was identified as a precursor lesion in the tubal epithelium. Additionally, the concurrent presence of identical somatic TP53 mutations in STIC and pelvic HGSC lesions support this establishment. Furthermore, gene expression in HGSC is more closely related to fallopian tube morphology than to the ovarian surface epithelium. HGSC expresses a Müllerian marker (PAX8), not a mesothelial marker (calretinin) [3]. Bachert et al. [4] found that STICs have shortened telomere lengths compared to those in normal tubal epithelium. HGSCs are longer than their counterpart STICs. STICs are precursors to HGSC because telomere shortening is a known early event in the neoplastic transition.
The incidence of STIC ranges from 0.6–6% [5]. Approximately 10–15% of STIC lesions are detected in women undergoing RRSO for BRCA 1 and 2 mutations. STICs are detected in approximately 50–60% of patients with sporadic pelvic HGSC [5].
In our cases, the patients were not examined for BRCA mutations because they had no familial history of cancer. Few reports have described incidental STIC in patients with unknown BRCA mutation status. Although its prevalence has not been established in large studies, the STIC frequency in these women is 0.6–1.1% [6]. The reported median age at the time of incidental STIC diagnosis during surgery for benign disease is 61 years (39–86 years) [7].
There are no standardized criteria for STIC diagnosis because the histopathological spectrum is very wide. Currently, most STIC lesions are diagnosed using a combination of histopathological and immunohistochemical staining [5]. The Sectioning and Extensively Examining the Fimbriated End protocol has been developed to detect STICs more reliably [4]. STIC is characterized by secretory cell lesions with some degree of cellular depolarization, increased nuclear-to-cytoplasmic ratios, hyperchromasia, nuclear molding, prominent nucleoli, and increased mitotic activity [4]. Staining of p53 (overexpression or null phenotype) and Ki-67 support the diagnosis of STIC. p53 staining revealed complete loss in the suspicious areas in the first case and focal positivity in the second case.
As reports of STIC lesions are rare, data on the clinical outcomes and management strategies are limited. Wethington et al. [8] retrospectively evaluated 593 high-risk women who underwent RRSO with concomitant peritoneal washing. Twenty patients (2%) were diagnosed with STIC, of which 12 were isolated. Seven patients underwent surgical staging, and none of them had malignant pathology. The patients were followed-up with CA-125 estimation, imaging, and pelvic examination for approximately 28 months, with no recurrence [5]. Although the sample size was small, the study showed lower surgical staging and a favorable clinical outcome. Patrono et al. [9] performed a comprehensive review of the clinical outcomes and management of patients with incidentally isolated STICs. We recommend prompt BRCA mutation screening after STIC diagnosis. Van der Hoeven et al.10 described the staging procedures in 13 of the 82 patients with isolated STICs who underwent RRSO. None of the staging procedures reported metastatic or advanced disease, and the estimated recurrence risk was approximately 11% after a median follow-up period of 42 months. No recurrence was reported in patients with STIC at RRSO who underwent staging or chemotherapy. However, there is insufficient data to define the extent of the staging procedure and the need for re-operation after incidental STIC detection. Close surveillance, surgical staging, or empirical adjuvant chemotherapy are the available options, as there is no current consensus among gynecologic oncologists regarding the appropriate management of incidental STIC detection [5]. Staging surgery is recommended for patients with incomplete evaluation. However, these options may be controversial given the expensive subsequent studies that yield very low detection rates for early primary peritoneal cancer presentation. Given the possibility of adverse effects, the risk-benefit ratio should be discussed with the patient before initiating management. In cases of incidental STIC lesions without other invasive diseases and risk factors, follow-ups with the patient are a reasonable choice [10]. Follow-ups at 6-month intervals, including gynecologic examinations, CA-125 and/or HE4, and ultrasound examinations may be recommended. More studies are needed to assess proper management strategies, although these might be limited by small sample sizes.
Epithelial ovarian cancer is a leading cause of death, with the most fatal subtype being HGSC. As 80% of ovarian cancers occur in women with no known family history, the risk of fallopian tube and ovarian cancers should be considered in all gynecological surgeries. To date, no functional screening methods have been developed. Current modalities such as gynecological examination, transvaginal ultrasound, and serum CA-125 and HE4 biomarkers have not yielded satisfactory results [10].
In response to the gradually accumulating STIC studies, several providers have expanded the role of routine salpingectomy, hysterectomy, and sterilization procedures [4]. The Society of Gynecologic Oncology and American College of Obstetricians and Gynecologists suggest that opportunistic salpingectomy should be considered for women undergoing hysterectomy without cancer risk after childbearing to reduce the risk of HGSC [6]. Salpingectomy during benign pelvic surgery appears to be safe and does not increase the risk of complications. Additionally, the ovarian function is not affected by salpingectomy. Currently, there are no data either showing a reduced risk of ovarian cancer in the average-risk or inherited high-risk populations. Although it will take decades to demonstrate a change in mortality due to opportunistic salpingectomy, the effectiveness of salpingectomy will gradually increase, given the decades of research on STIC and HSGC. Appropriate physician-patient shared decision-making regarding adnexal management for benign hysterectomy should always be followed.
Various studies have improved our understanding of the association between STIC and HGSC. This recent paradigm shift in the understanding of extrauterine pelvic cancer has clinical implications for its screening, prevention, diagnosis, and management [10]. Early detection is a key factor in overall mortality reduction; however, there are no reliable tests. Salpingectomy during benign surgery may be an alternative strategy to reduce the incidence and death rates of ovarian cancer in the general population [10].
Currently, no clear guidelines exist for the management of incidentally identified STIC. Patients should be evaluated for risk factors including BRCA1 and BRCA2 mutations. Careful decisions should be made regarding additional surgery, adjuvant treatment, and follow-up plans considering individual patient factors.
Acknowledgements
This work was supported by the education, research and student guidance grant funded by Jeju National University